- HOME
- ABOUT US
- WHAT IS AiARTHRITIS
- Diseases
- Rheumatoid Arthritis (RA)
- Psoriatic Arthritis (PsA)
- Systemic Lupus Erythematosus (SLE)
- Sjögren's Disease (SD)
- Axial Spondyloarthritis (AxSpA)
- Crohn's Disease
- Sarcoidosis
- Relapsing Polychondritis (RP)
- Systemic Sclerosis/Scleroderma (SSc)
- Behcet's Disease (BD)
- Palindromic Rheumatism (PR)
- VEXAS
- Antisynthetase Syndrome (ASS)
- Mixed Connective Tissue Disease
- JIA
- Familial Mediterranean Fever (FMF)
- HIDS (hyper-IgD syndrome, a mevalonate kinase deficiency)
- Cryopyrin-Associated Periodic Syndromes (CAPS) - Familial Cold Autoinflammatory Syndrome, Muckle-Wells Syndrome
- Schnitzler Syndrome
- Chronic Nonbacterial Osteomyelitis (CNO)/Chronic Recurrent Multifocal Osteomyelitis (CRMO)
- Still's Disease
- All Diseases
- Diseases
- OUR WORK
- RESOURCES & TOOLS
- GET INVOLVED
- CONTACT US
Psoriatic Arthritis (PsA)


How to pronounce it:
Psoriatic - So-ri-at-ic
Arthritis - Ar-thry-tus
AiArthritis defines psoriatic arthritis as:
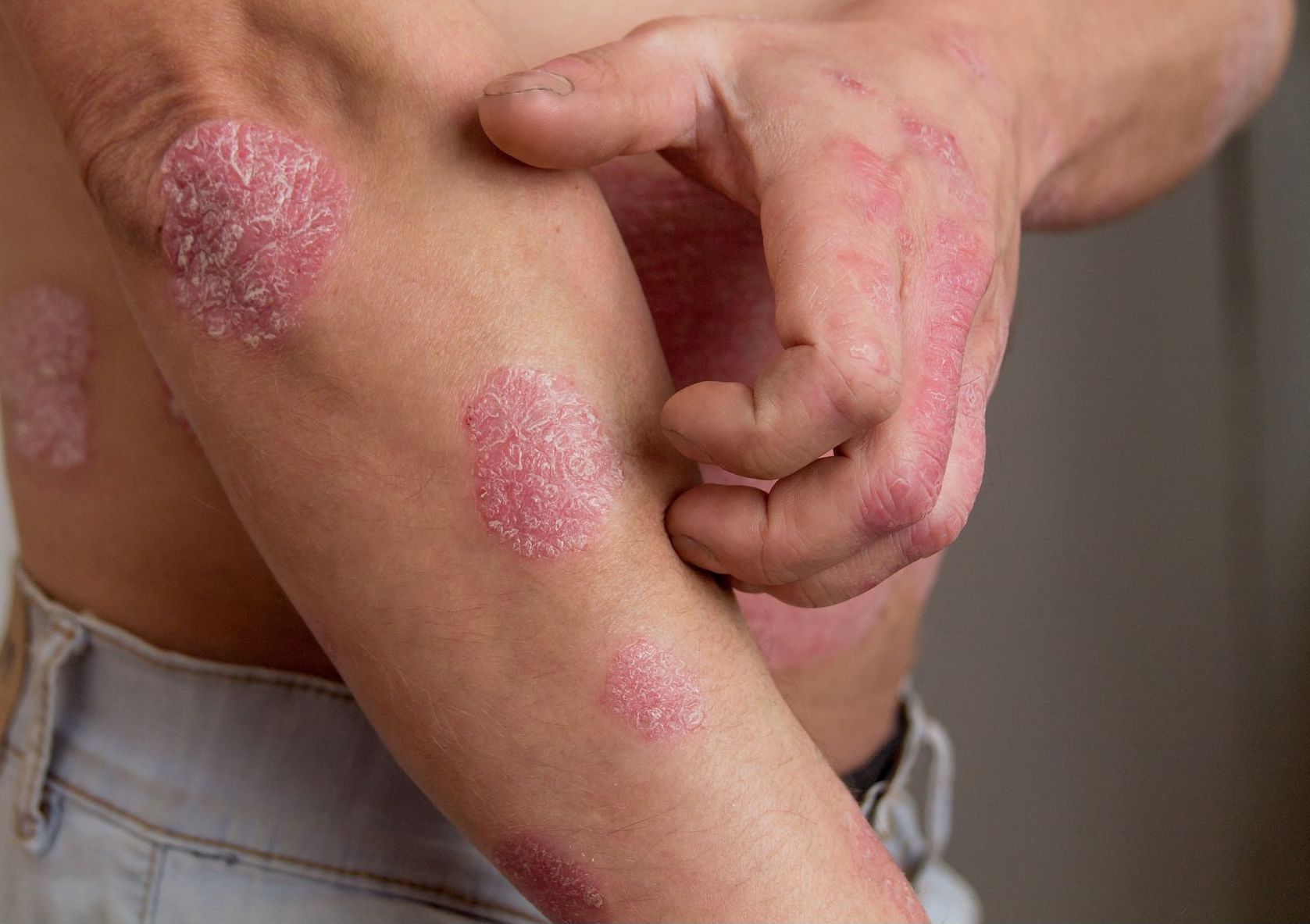
Psoriatic arthritis (PsA) is a chronic, inflammatory disease that in addition to joints often causes enthesitis (inflammation where tendons and ligaments connect to bone) and often affects the organs (skin, eyes). Psoriasis rash is usually present, but it may not be visible (on the scalp) or may not present for years after onset.
- Juvenile version is Juvenile PsA
Symptoms
Symptoms of AiArthritis Diseases Regardless of Diagnosis


Common in All AiArthritis Diseases
- Periods of worsening symptoms are called flares. A flare can last for hours, days, weeks, or months.
- Condition improves with activity and exercise and worsens with rest.
- When inflammation is left uncontrolled due to lack of proper treatment, comorbidities can develop. 70% of patients with chronic, lifelong disease will develop comorbidities, including dual or triple diagnoses.
- Autoimmune diseases run in families. If anyone in your immediate family (parents, siblings) or extended family (aunts, uncles, grandparents) have been diagnosed with ANY autoimmune disease, there is the possibility of genetic predisposition.
Typical “Auto” Symptoms
- Severe fatigue or exhaustion that may not be helped by caffeine/stimulants and can happen even after a long period of rest.
- “Brain fog” - or periods of time where thinking gets clouded and it becomes difficult to concentrate.
- Flu-like symptoms, without having the flu- nausea, muscle weakness, and general malaise.
- Fever, typically low grade in autoimmune (with exception of juvenile idiopathic arthritis) and higher grade in autoinflammatory (% strongly varies per disease).
Reference: Early Symptoms of AiArthritis Study, AiArthritis, 2019.
Typical Arthritis Symptoms
- Severe stiffness in one or more joints, especially in the morning or after sitting for long periods of time.
- Episodes of joint pain that may last for hours, days, or even weeks, that can appear and disappear suddenly. Often described as “jumping pain” into different locations.
Typically the joint pain will coincide with one or more “Auto” symptoms and start and stop suddenly - for no apparent reason (which is called a "flare"). Some people will experience all of the above symptoms, others only a few. If you have any of the arthritis features, and at least one of the “Auto” features, please consult your physician about a referral to a specialist.
Symptoms Often Associated with Psoriatic Arthritis:
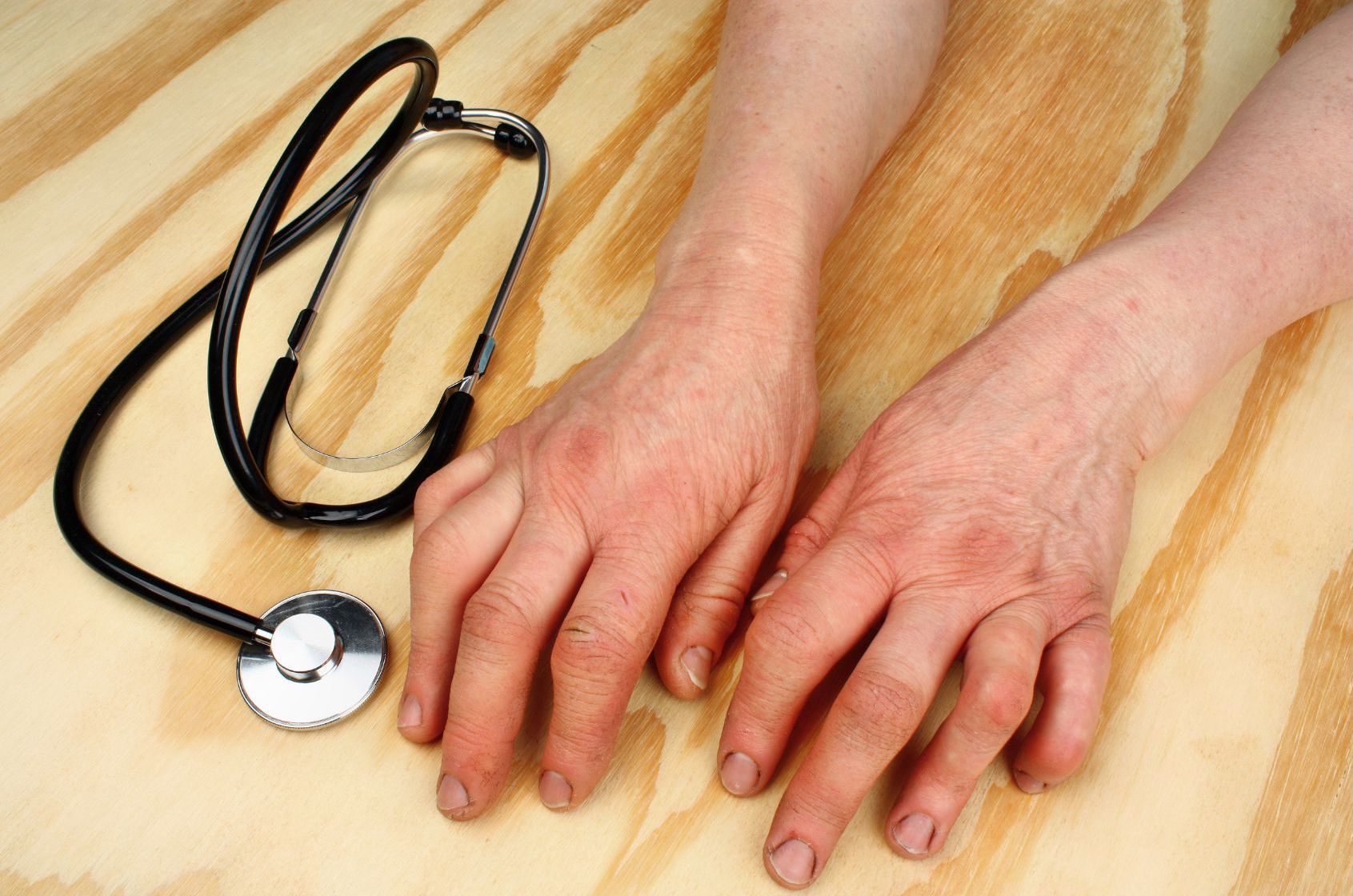
- Swelling of an entire finger or toe, sometime causing a “sausage” like appearance
- Sometimes one entire, individual finger or toe will swell up, making it painful and hard to bend (called dactylitis)
- Psoriatic skin lesions that itch and can be painful (not contagious!)
- Enthesitis, which is inflammation in places where ligaments and tendons connect with bones, such as at the Achilles heel in the foot, legs, or chest
- Usually accompanied by symptoms in the fingernails and toenails, ranging from small pits in the nails, cracking, white spots, crumbling, and sometimes the nail can separate from the nail bed
- Some people develop back pain and stiffness, primarily in the lower back, neck, and upper back (spondylitis)
What fellow patients want you to know

It may be confusing to get a diagnosis of Psoriatic Arthritis and NOT have psoriasis, but it could happen. It's also possible to have psoriasis and no one asks if you have other symptoms that could lead to a psoriatic arthritis diagnosis.
Nail changes are visible. If you paint your nails or wear fake nails, try not doing this for awhile to see if you have nail changes (like ridging, breaking/cracking).
Even though it's called Psoriatic Arthritis, and often joints are part of it, enthesitis - or the tendons where it connects to your bones - are usually involved. This can be in the feet (often heels), chest (called costochondritis), spine and more. with dandruff.
Keep an eye out for small patches of psoriasis that may be hidden (like scalp), which could be confused with dandruff.
More About Psoriatic Arthritis
Diagnosing Psoriatic Arthritis

There’s no single definitive test that can confirm a diagnosis of psoriatic arthritis (PsA), so rheumatologists look at a combination of physical exam, blood tests, and imaging (x-ray), along with a family history of autoimmune or autoinflammatory disease.
During the physical exam, the rheumatologist will check for pitted fingernail and skin lesions that may be caused by psoriasis. The doctor will look for any other signs of psoriasis accompanied by sore or swollen joints.
The blood tests will test for C-reactive protein and rheumatoid factor (RF). Most people with PsA are RF negative, if the person is RF positive, the doctor would likely explore a Rheumatoid Arthritis (RA) diagnosis instead.
If you get x-rays, they will often scan hands and feet for damage. PsA may have a type of damage not seen in other types of AiArthritis diseases. However, keep in mind often x-rays will not be sufficient to show damage and often require MRI or other type of imaging.
They will see if the arthritis is in more than one location and if it is chronic (has lasted for more than 6 weeks continuously or has come and go during that time).
The doctor will look closely at the joints to see if there is any swelling, redness, or warmth (although this isn't required for diagnosis - it is more to see the severity). They will also screen for enthesitis, inflammation of tendons around the bone, which is more common in spondyloarthritis diseases.
Most rheumatologists today will also consider if you are feeling other common symptoms (see Common Symptoms in All AiArthritis Diseases), which can help differentiate from any other diagnosis vs. an AiArthritis disease.
Notable Persons with this Disease

- Kim Kardashian, Reality TV Personality
- Phil Mickelson, Professional Golfer
- Dax Shepard, Actor
- Stacy London, Reality TV Personality
- Ted Danson, Actor
- Lance Bass, Singer
Interesting Facts about this Disease
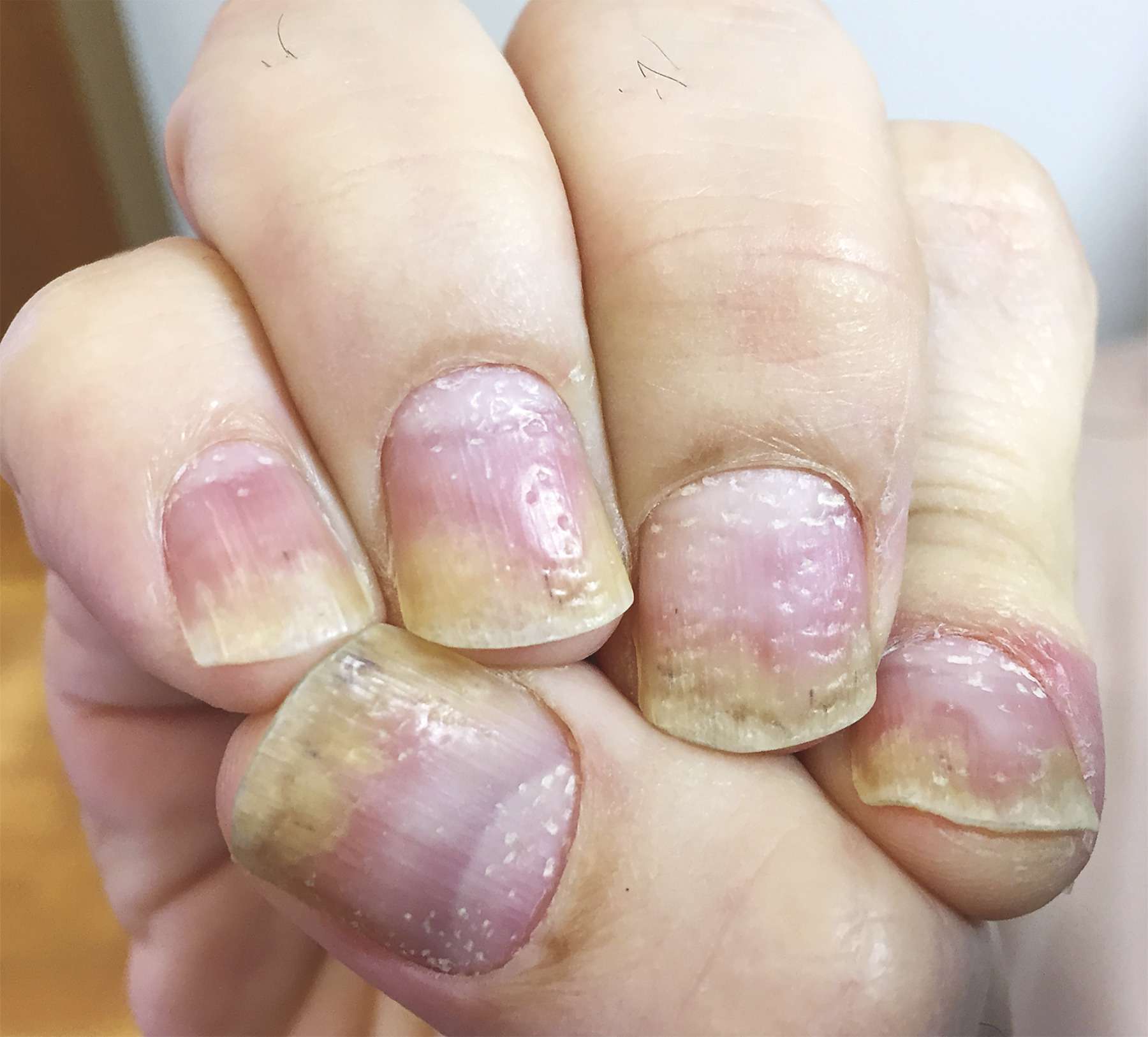
- More than 85% of people who have psoriatic arthritis also have nail psoriasis
- 30-33% of people with psoriasis develop psoriatic arthritis
- The severity of one's PsA isn't directly related to the severity of one's psoriasis
- Precision Medicine - Genetic markers including HLA-C, IL128, TRAF3/IP2, FBXL10, and IL23R may be associated with Ps/PsA
In an effort to ensure this page has the most accurate and up-to-date information, this page is currently awaiting medical review. Some information is subject to change.
Page Last Updated: 2/1/2023
Sign up for our newsletters
International Foundation for AiArthritis
6605 Nottingham Ave.
St. Louis, MO 63109-2661
Toll Free: 1-877-609-4226
Text: 1-314-282-7214
Copyright 2024. All rights reserved. Information on this site is intended for informational purposes only Our foundation does not engage in the practice of medicine. Please consult a physician to obtain personal healthcare and treatment options. 501(c) 3 Nonprofit Tax ID: 27-1214308.


