Ep 119: What I Wish I Would’ve Known After Diagnosis
AiArthritis Voices 360 Main, Full Episode 119
Air Date: March 1st 2026
This episode is a step 2, as outlined in our 6 Step Patient-Led Problem Solving Process.
A new diagnosis can bring relief, fear, and uncertainty all at once. In this episode, Leila and Deb share advice from the AiArthritis community on what they wish they had known right after being diagnosed with an autoimmune or autoinflammatory arthritis disease.
Leila and Deb explore the importance of trusting your body, especially when tests are inconclusive or symptoms are dismissed. This episode highlights how self advocacy, second opinions, and clear communication with your care team can shape your experience. Community members also reflect on the emotional side of diagnosis, including grief, patience, and the mindset shift that comes with learning to live with chronic illness.
Whether you are newly diagnosed or supporting someone who is, this episode offers validation and practical guidance for navigating the early stages of the patient journey.
Episode Highlights:
- Why trusting your body matters, even when tests are unclear
- How self advocacy and second opinions can change your care experience
- The emotional impact of diagnosis and the importance of grace and patience
- Practical tools like symptom tracking, rest, and shared decision making to support long term management
Have questions about this episode or topics you want to hear us bring to the table?
Email us at podcast@aiarthritis.org
Donate to Support the Show: www.aiarthritis.org/donate
AiArthritis Voices 360 is produced by the International Foundation for Autoimmune and Autoinflammatory Arthritis. Visit us on the web at
www.aiarthritis.org/talkshow. Find us on Twitter, Instagram, TikTok, or Facebook (@IFAiArthritis) or email us (podcast@aiarthritis.org). Be sure to check out our top-rated show on
Feedspot!
Follow AiArthritis on all social media platforms
-
Episode 119 Transcript
AiA 119 Podcast
===
[00:00:00] Welcome to AiArthritis Voices 360, the podcast solving today's most pressing issues in the AiArthritis community. We invite you all to the table, where together we face the daily challenges of autoimmune and autoinflammatory arthritis. Join our fellow patient co-hosts as they lead discussions in the patient community, as well as consult with stakeholders worldwide.
To solve the problems that matter most, whether you are a loved one, a professional working in the field, or a person diagnosed with an AiArthritis disease, this podcast is for you. So pull up a chair and take a seat at the table.
Hello and welcome to AiArthritis Voices 360. This is the official talk show for the International Foundation for Autoimmune and Autoinflammatory Arthritis, or AiArthritis for short. My name is Leila P.L. Valete, [00:01:00] and I am one of your co-hosts. Today I'm a person living with Lupus and Sjogren's Disease and I am the health education manager here at AiArthritis.
And today I am joined by one of our long time. Superstar volunteers, Deb Stein. Deb, if you wanna introduce yourself a little bit. Absolutely. Hi everybody, I'm Deb Stein. Um, I live in the state of Wisconsin and I have had RA since I was 13 years old. So 43, 44 years of, uh, journey and, um, so many.
Comorbidities that have joined the, the, the pile of things that I have, as well as newly diagnosed with Sjogren's as well. So yeah, here we go. So newly diagnosed can, can really be at any part of the stage in your journey because of [00:02:00] how common it is for autoimmune diseases to compile. Um, once you have one, it's very likely that you do, you will develop another.
And so both Deb and I were newly diagnosed with Sjogren's after having our respective diseases of lupus and RA for a long time. So we had to go through the newly diagnosed phase. A few different times. Um, but we kind of have similar stories as well in terms of how early we were diagnosed because I was actually diagnosed at 12 years old as well.
So maybe some of the challenges that we, um, may talk about in the rest of this episode, um, didn't apply to us at that time of our initial, um, diagnosis because. We were still growing and, and understanding who we were as people. But the second time around, definitely, uh, I'm like, yeah, there's a lot to, to learn when you have a new disease that's on the horizon.
So, you know, that's leading into exactly what we're talking about today. The topic is what I wish I [00:03:00] would've known after diagnosis or when I was newly diagnosed. And so, um, this is a. It's a, it's a topic that we've talked about several different times on the talk show. Um, a lot in the early days, um, of the talk show.
There was actually, um, an episode where, uh, um, I think it was a mini episode where Tiffany talked about, you know, who am I now? Yeah, once you were diagnosed, um, a lot of people, especially when they're diagnosed in their adult years, it, it's really a shock when it comes to, to getting that diagnosis and how much your life has to change and it, and I suppose all the things that, um, happen that you need to change in your life, whether you like to, you want to or not.
Yeah. And sometimes, you know, people can, can jump in and do it all at once and sometimes it's a. Really slow progress of being able to, um, change all of those different things that can help with your diagnosis. And [00:04:00] just even learning to take medicine every day or going to your infusion once a month, whatever it may be.
There's no shame in it being such a tough. Um, thing to overcome, but it is also important to know that you're not alone. A lot of people have gone through the same feelings, the same situations, and so that what we're here to talk about today. So, uh, we're, we basically collected, um, advice from patients over the past year or so.
Um, we have a, we had a form on our website that was. Asking patients to tell their own diagnosis story and also any advice that they would have for those who are newly diagnosed and not to any surprise. Um, the biggest theme that we saw here was advocacy, advocating for yourself, being informed and making sure that you are able to educate sometimes to, uh, your primary care doctor, to the emergency room doctors.
Just being [00:05:00] able to, um, you know, talk about your disease and how it's affecting you. Um, because many, many, many healthcare practitioners and people in the world are not educated about these diseases. Agreed. A hundred percent agree. And it, it is. Something that is interesting about how you have to take that on.
And here I am at 56 years old and my son, who is 26, shortly to be 27, he was diagnosed, um, a little over two years ago and it's a different ball game again. When I was a child and you were a child. I remember my parents not sharing information with me, and I'd walk in on them and they'd all be crying and the discussion would stop and they wouldn't share with me, and [00:06:00] that's one thing.
I think it was protective on their parts. I did not like that. And I think, you know, if you're talking about me, you can't talk about me without me. So definitely, I think that was one thing in particular. But, um, seeing things through my son's eyes has been enlightening as well. And I'll share at some point.
The comments that he shared about, he even talked about even before he was diagnosed, what he wished he would've done so and after at this point. So it's kind, it's interesting. Everybody has a different, um, journey and every journey's okay. It's the way you need to handle it. Exactly, and for me, when I was newly diagnosed at 12, I didn't have a lot of major symptoms that were happening.
I was diagnosed really early in the development of my [00:07:00] lupus, so I'm very lucky in that sense that that had happened, but it also made me really, it made it really easy for me to ignore. What was happening for a very long time. Yeah. And so I didn't identify as someone who had an autoimmune disease or someone who had lupus.
It was very like, oh yeah, that's something that I have, but it doesn't really affect me. I take medication. Um, a lot of people just didn't know that about me because it wasn't something that was, um, actively happening in my life until it was actively happening in my life, which happened at 18. I got a viral infection and that really pushed my symptoms too.
Forefront and when everything started happening. So I guess I've had had this newly diagnosed situation happen three times where, or even four times where it was the initial diagnosis and denial and then finally having to address, oh, I have these symptoms and this is really happening to me. Then developing lupus nephritis and all of that had to do [00:08:00] with, because.
Lupus, SLE versus lupus nephritis is a whole different ballgame when it comes Yeah. To kidney involvement and, you know, potential for need of dialysis and things like that gets really scary. And then the addition of Sjogren's right after that as well. So, um, we go through this in stages. It's not something that just happens once really when it comes to these disease.
Disease unfortunately. Yeah, for sure. Because again, my. I was perfectly fine until I had a foot surgery and I came home full blown. So it hit hard and like a lot of things had to come to stops. Like I was on a swim team and I played flute and I couldn't do any of those things anymore. So some of those things, um.
It hit hard and if there was ever a depressed [00:09:00] time in my life, it was probably during that time and you know, starting medications that didn't work very well and had horrible symptoms and. Had to stay home many days 'cause I couldn't even get out of bed and all those things being freshman year of high school, bam.
Yeah. Craziness. And it's, it, it really does, like you said, affect everybody differently. And so, yes. So the first thing that we, I wanted to talk about is one of the themes, um, that we saw on some of the, um, submissions that we got. Um, one of the biggest things is. No, you're not crazy. Make sure you trust your body.
And I think, you know, getting that diagnosis finally can help with validating the fact that, you know, you probably thought that you were crazy. It was all in your head. There's, you know, all of these different doctors telling you different things before the actual diagnosis happens. And once [00:10:00] the diagnosis happens, you're like, oh my goodness, thank God.
Like I knew I wasn't crazy anymore. But then it flips right away and you're like, oh crap. I, I actually have this disease. Yeah. And what does that mean now? Yeah. Because I remember, um, people get the feeling that they, or people are telling people that it's all in your head. And then you start to think that you are crazy.
And I mean that it takes you down a whole different path. And like you've said, it's an invisible disease in many cases that people are like. You can't feel that bad, right? No, exactly. And um, there, one of the quotes that is pulled from a submission, it says, the hardest part was being told nothing was wrong with me as nothing showed up on the tests.
Right. And that is a such a common occurrence that happens all the time. And what [00:11:00] we're seeing now, um, in the research side is that. Some, for a lot of the diseases, these biomarkers in your blood don't actually show up until the disease is a little bit further in, in progression. Um, so that, and it's five years for me until all my lab started showing things, but.
We knew some symptoms start first. Yeah. Yeah. And my son, I think, helped him get diagnosed sooner was the fact that I had RA and they went down other paths. 'cause his labs still are pristine and perfect. So, um, had he not had a mom with ra, he'd still be sitting in la la land and not Yeah. Being on medications that are helping him.
And really, um, are stopping the progression of the disease Yes. To, to happen even more so. Yes. And so that's, that is also, you know, super important to, um, to know it is. That's, you know, [00:12:00] we call this seronegative when, you know, things are not showing up in blood work, but you are still having symptoms. Yeah.
And we're, you know, the paradigm is starting to shift where. You know, we're trying to get rheumatologists on board to diagnose based on symptoms and not based on imaging and blood tests, because we're now seeing that even with these, um, you know, tests being pristine. Yep. Many of these people are, do, have active disease and it's, it's really crazy though that it doesn't show up on the inflammation markers.
Like, it, it doesn't make sense to me or. I know, and it's, it's frustrating, um, for everybody involved because the doctor wants, you know, they wanna help you no matter what. If you're having these symptoms, their goal is to help you, but they also don't wanna give you medication that you maybe you may not need if there's not any evidence to show.
So, um, yeah, that's, that was one of the big themes that, um, we saw is, you know, just. Once you get the diagnosis, [00:13:00] you know, trusting your body, knowing that you know what's going on in your body, um, it may take you, you know, some time to learn your patterns. Yeah. But once you do that, that really is kind of empowering so that you can know that, you know, I know what's happening in my body and I knew this whole time.
Yep. For sure. Okay. So that also leads into, once you know you, what's going on in your body and you trust yourself that, you know, that's when you can really start to advocate for yourself. And, um, adv advocacy really does make a difference, um, because although the doctors are the experts in medicine, you are the expert in your body and what's going on in your body, and you're the only one that can explain that.
So just, you know. Really, you know, saying what's happening in your body. Even if one doctor dismisses it and says, oh, that's, you know, it, you know, that might be happening because [00:14:00] you're using, you know, you're typing too much. That's why your hands are hurting. Or, you know, any of the other things that may be written off.
Um, continuously Change of weather. Change of weather, yeah, weather, because I'm going through something right now and I'm already three months into it and I have. All different doctors looking at me being my primary care, my rheumatologist, and um, eye doctors, ophthalmologists, and I was first told, oh, that might be just because of the change of weather and you're turning your heat on.
No. So I, I, I'm living that right now, and I am, I'm fighting hard and it's good to talk about it with other people because I, even today, Leila and I were chatting about it and she gave me another option to, you know, seek out. So I think that's my next point on my path. Yeah, and I think that, that, that's, it's really hard because.[00:15:00]
We're not seen as a, as an authority. Um, you know, we're not the experts and so it's, it really is, it takes a lot of, uh, confidence and advocacy for you to kind of push back on the doctors sometimes, because we are taught that, you know, doctors, you know, are, they kind of know all, and you know, whatever they say goes.
And, you know, in a lot of cases that that is the case. You know, if they're a brain surgeon, I have no idea. Go ahead, go ahead and tell me what I need to do. But when it comes to these chronic illnesses, it really does become like a shared, um, a shared expertise with your, your rheumatologist and with yourself.
Um, because there's just so many different things that go on. So, yeah, advocacy is, is so huge. Um, some of the quotes that are here, um, says, do not take no for an answer. Keep fighting. Do not allow gaslighting of your symptoms, which we [00:16:00] just talked a little bit about. Yeah, it's due to the weather, it's due to, you know, any other, um, things that may be going on.
And of course, request a second opinion if you feel someone is dismissing you and. You know, unfortunately in our healthcare system, sometimes that's not, um, as easy as we, we, we wish it could be. Especially if you're on government, um, assistance, um, insurance like Medi-Cal or even with Medicare, um, they gotta give you really stringent guidelines of who your doctors need to be.
And that's, and it's, it really is. Um, it's a tough situation. Um, but one, one way that you can, you know, maybe seek some, uh, second opinions is being a part of any of these patient organizations like ai, arthritis. Um, you know, autoimmune Association, arthritis Foundation, um, all of these different organizations, they will have webinars with experts on them that you can ask questions to, [00:17:00] that you can, um, seek out and, you know, maybe send an email to about your specific situation.
Um, because yeah, it's really, it's really hard to just really, um, stick with the opinion of one person when they, when you feel like they're dismissing their percent. Yes. Yeah. Sorry, we're going through it right now, so, exactly, yes. And um, one. Okay. The next set of. Submission, uh, themes is addressing the fact that, you know, there is grief that happens when these diagnoses, um, occur.
Um, a lot of patients is needed and there's a mental shift that needs to happen and that kinda happens on a different timeline for everybody. Um, you know, have to go through the stages of grief, right? Like with anything that, um. You know, you're mourning the, uh, existence of what your life was beforehand and what it needs to [00:18:00] be now.
Um, and that can be really tough. I know my son has gone through a lot of that. Um, he's a personal trainer, so he's still moving a lot and, um, he does have better days than others and is pushing himself to try to demo things for clients. All of those things can, it's, it is trying to have patience with yourself and, um, just being patient through the different things that are happening in your life.
Um. Maybe now is a time that I could share what my son's comment were. Yes. Um, I reached out to him and asked his opinion and, um, he thought about it all night and got back to me this morning. He even went to before diagnosis, um, he said, I wish I knew a little bit more about different substances and tech.
Sneaks that I could have done during my athletic years to increase my joint stability, [00:19:00] to prevent my meniscus tear that begun the diagnosis pattern for him. And after, um, he said in addition to the medications, he said finding all natural foods that can help with inflammation and joint stiffness. So he's definitely is looking into all the different protein powders and how things affect him and just doing more just really.
Paying attention to what he's eating and not eating junk as much, or soda or any of those type of things. He's trying to cut back on those things, which he says has made a big difference in his inflammation in addition to his pen injectors. Definitely and, and for everybody, um, you know, the, the diet can, can be different and can change depending on how you react to it.
But generally what we recommend [00:20:00] and what we have a lot of resources on is an anti-inflammatory diet. Yeah. Um, you know, sticking to, you know, all the, the great, um, amazing healthy fats. Fish, um, you know, lean proteins, um, staying away from, from red meats as much as possible. Um, kind of like a Mediterranean diet is, is what, um, is called as well.
Lots of legumes and, um, all of those other sources of protein as well. And of course, lots of fruits and vegetables, minimal amounts of carbs. Um, there's lots and lots of resources out there, um, including from ai, arthritis, and any other people that are in the community. A few off the top of my head that I know of is, uh, Christina Montoya, who is the arthritis dietician.
Um, at arthritis Dietician, she has lots of amazing, um, recipes and resources as well as Tanya Fred Rich, who's also the lupus dietician. She has amazing, um, resources on, um, [00:21:00] diet as well. And so, um, I think that is one of the, um. The biggest, there's lots of, um, resources in the community and both of those, uh, people are also patients themselves.
Um, so they are, uh, amazing resources to take a look at. Um, I actually got a, um, video submission from a patient, um, her name is Heather, and she also talked about how much. Changing her diet really helped and it made her feel more in control as well because she knows, you know, that the stuff that she's putting in her body is, is helping, um, her inflammation.
And, um, there's some very specific. Types of food that she mentioned, um, that I can kind of put in the, in the footnotes here of the episode, um, for you all to check out some information about it. But diet is, is a really big one as well as exercise for sure. Um. I know that, um, I'm a medically retired dietician, so [00:22:00] again, I did all the research into everything and I tried the elimination diet to see if I had any food triggers.
Of course I didn't, but, um, I, I do mostly follow the. Um, anti-inflammatory diet and it does make huge difference. I used to drink lots of soda every day. Um, big bottles of Dr. Pepper was my beverage of choice. And, um, I've cut out those things and I do feel better. So. Making better choices and really cutting back on the greasy fat foods.
It does help in the long run. And my son has even commented that he's working on that and his thing is motion is lotion, so. Mm-hmm. He, with all the ex exercise he's doing is really important. And that's what, again, with all of the research conferences that we've been going to, um, there's a lot [00:23:00] more about exercise and how much it actually really does help.
And it's a little bit counterintuitive when you think about it because of how much pain we're in. But really it is about, yeah, loosening up your, your joints. Getting them warm, getting them, um, you know, up and moving can really help with actually the pain. Um, because you're moving around those synovial fluids that are in your joints, um, that maybe help like, you know, get, cause the inflammation, the lactic acid, all of those different, you know, things that happen in your joints that can, um, cause inflammation if they just sit there and kinda stay there.
So. We, we also do have some resources on exercise, um, as well on our website that I can link in the, uh, description here for the episode. You've done a fabulous job creating these documents that are very patient, friendly and usable, that anybody of any like education level can [00:24:00] easily understand and follow.
Some easy things that you can do at home every day. Yeah, it's been a huge, uh, project over the past year to build out this patient journey Yes. Resources and it's, um, there, yeah, there's a lot that's out there. One of the biggest sections that we have is called disease management, so that's one of the stops on the patient journey.
And that's where all of, a lot of these resources, um, that are non-pharmacological, um, interventions that you can look into and, and help improve your, um, your quality of life. Although it's very, very obviously recommended and, and needed to have those, um, medication that are helping to, you know, slow down your immune system.
And, um, you know, kind of stop the inflammation systemically. There are so many other lifestyle things that you can do to also aid and help those things. Like, like diet, exercise, acupuncture, chiropractic, massage. Yes. All of [00:25:00] these different things and adapt. D tools, compression gloves, all of these different things that can help to improve your quality of life even more so, um, a a additionally to sticking to the treatment plan that, um, your rheumatologist, you know, gives you.
But yeah, also a bunch of, um, things in the kitchen. 'cause I love cooking and, um, different things that can actually help. I will say sharp knives make a big difference. Yes. And my husband, um, sharpens our knives probably at least four to six times a year. And, um, when he is got a little extra time, he's got a, um, a tool out in the garage and he.
Just takes up all out and five minutes later he is back in and they're all good and sharp and um, I have a bunch of things for chopping onions and. Um, squishing garlic cloves that are easy. Just a twisting motion [00:26:00] versus trying to squeeze the garlic press 'cause my hands are awful. And, um, I found several other tools that work fabulously and like work simplification for the most part in the kitchen.
I've got lots of tools. Yes, we, um, in our anti-inflammatory diet resource and there's actually. A whole page that, um, Deb had given us, um, on some of the adaptive tools that she uses in the kitchen. So that's one of the resources that I definitely will link here. That, um, is actually one of our most popular downloaded resources, which is a, um, it was a community chat with me, Deb and Christina Montoya, who I mentioned earlier.
Um, and that it, it literally is probably our most. Downloaded resource right now on our website. And so, um, it's really great to see the community really wanting to make a difference in their, in their disease journey with, um, all of the different, um, diet tips. It's great to [00:27:00] have those type of things because it's expensive to eat out.
So that was my one big thing of trying to make it easier in the kitchen. We talk a lot about, um, frozen, frozen produce, um, and canned produce and things like that in that, uh, in that resource as well. So definitely that's what something that I've been using is a lot of frozen vegetables because vegetables go bad so easily.
They do. They do. And so the last section of um. Things that I wanted to talk about is, uh, other helpful tips just for those who are newly diagnosed and we went into diet and exercise as, um, you know, how important that is. Um, and the next thing is, um, sleep and rest is just as important. And, um, I know that it sounds like a lot when they say that they recommend eight to 10 hours for those who have autoimmune disease.
But if you think about it, our cells need to repair a lot more than other people's cells need [00:28:00] to repair. Um, our cells are constantly, our, our antibodies are constantly fighting against the cells in our body. And so cellular repair, um, happens when you're sleeping and it's really important to make sure that you get enough rest.
It, it's tough to do so sometimes because there's also this phenomenon of pain, insomnia, where if you are in so much pain it can cause you to not be able to sleep well. So get getting some interventions from doctors on, on how to sleep, um, get more quality sleep is, um. Is, is something that is really important as well for me.
Um, something that I use is magnesium glycinate. Um, that helps me to kind of relax and rest at the end of the night and get more quality sleep more than even like melatonin. Um, I feel like melatonin has, it was very popular for a while and is kind of, uh, people have kind of been, um, stepping back from it a little bit because, um, there are, you know.
Some other, uh, [00:29:00] consequences that may happen with melatonin because it's, it's kind of in interrupting your circadian rhythm. So it, uh, there's other more natural ways to help with, um, getting more quality of sleep. A lot of people recommend chamomile tea at night. Um, and there, you know, when needed. There's also medications that doctors can prescribe you to help with that at night as well.
I will say being, um, definitely a lot older than you, Ms. Leila. Um, when. I mean, I get up probably two to three times a night to go to the bathroom and um, that definitely interrupts your sleep. Luckily, I'm usually able to fall back asleep. But one thing also is I, I go from shoulder to shoulder, so I am switching sides 'cause my shoulder cert.
But there, you know, like the t that is something that kind of just starts to help. Just relax your body. And I [00:30:00] think the warm, you know, like people used to say warm milk helped peoples. Mm-hmm. But I think the tea and chamomile and um, something without caffeine obviously is much better to drink at nighttime and a lot of those things.
But being a little bit older, you go through other, other changes in your body. Too. So, um, it's just always trying to keep up on it and just get the best sleep. And sometimes power naps during the day do help. Mm-hmm. Um, I occasionally will take those, um, if I'm really down and out, need the extra rest. Yeah, we're, um, there we're actually, you know, the US is one of the, um, cultures that doesn't really take naps, but if you think about it, like in Europe, a lot of people will take naps, uh, throughout the day.
And it's actually, I've seen studies that say that it's actually recommended for you to sleep in smaller increments than trying to sleep the whole 10 hours at what? Yeah. Yeah. [00:31:00] Um, so yeah, there they call, it's siestas. Yes, siestas in, in Spain for sure. My husband is actually one of those people that he has to re religiously sleep, um, take his nap in the middle of the day, um, because he, he can't stay asleep, um, for so long at night.
So he makes sure to take a nap instead of his lunch break at work, he will take a nap. So, um, is kind of my son too. So I wonder if it's kind of a male, male dominated thing that Yeah, maybe. Yeah. He also doesn't, my son doesn't go to sleep. Early, he sneaks up later as well. So yeah, he does get those naps during the day because it does make him feel better too.
Absolutely. Yeah. Um, and another tip that, um, you know, many seasoned autoimmune autoinflammatory arthritis patients will say is tracking symptoms and collecting data will really help [00:32:00] with treatment decisions. Um, you know, throughout your time that you have your autoimmune disease, there may be several times that you need to switch medications, um, switch up what's going on, depending on how your body is responding.
Tracking symptoms during those times can be very helpful in making sure that, you know, you're, the medication that you're choosing is, is the right one for you, and you and your doctor can make that decision more informed, the more data that you have, um, on your symptoms and how long these things have been going on, um, et cetera.
I definitely think that, um, over the years of being a patient, I have gotten really good at describing my pain and describing symptoms because I know that it's so necessary. And, um, if you're in pain, all the different [00:33:00] adjectives that describe. Pain alone. Um, burning, stabbing, throbbing, all those different things.
'cause it is very different, you know, as far as the kind of pain too. 'cause there's so many, there's several different kinds of pain that you can experience. Yeah, we, um, there was a eular, uh, yes. A eular, um, session. Was it last year? I don't think it was this year. I think it was last year. It was last last year.
Yeah. Yeah. When we were talking about the nociceptive pain Yeah. And all the, the, yeah. The, yeah. Neuroplastic. Yeah. There's so many different types of pain and the like, the way that you describe it can help just, you know, the doctors figure out which wines. You, you were talking about. 'cause there's the mechanical pain that's, you know, yes.
From wear and tear, from, you know, moving, um, too much and your joint's just breaking down. And then there's pain that's caused through the nervous [00:34:00] system and that's totally different. Um, so that's more like the shooting pain and things like that. The burn. Yes. Burning, yes. So that's total. It, it, it is, it makes a total difference on, again, um, making those.
Decision, uh, treatment decisions. So yes. Um, yes. And lastly, but definitely not the least. This is something that is super important that. May we talk about all the time and we, we hear this word, this buzzword and, um, it really is very important, but shared decision making and staying educated about your disease and, and, you know, updated on, on new treatments or any new research that's coming out, um, can really help you feel more in control.
And I think, um, those, for those who are newly diagnosed. That's something that they say a lot is that, you know, you just feel like you, your life's being taken over and you don't have control of what's going on because of the disease and taking these decisions and, and, [00:35:00] and, um, being informed can really make a difference in feeling how in control you are when it comes to these diseases.
I a hundred percent agree, just keeping yourself informed. Um, and I will say that AiArthritis is a reputable location to come to look for information on your disease type because we always use, um, science based information and based on data and research. There. If you're trying to Google online, make sure you're really careful about where you're going for your information because there's many, um, sites out there that are looking for money more than anything else.
So just, um, know that arthritis is reputable information that you're getting. Definitely there's a lot of, um, people out there that, um, advertise themselves as like health coaches for autoimmune diseases and things like that, and [00:36:00] they'll have information on their social media sites or their websites and things like that.
But you want to look to make sure to see if there's any reputable sites that they're citing. Mayo Clinic, Cleveland Clinic, um, the NIH, all of these different, you know, big sites as well as patient organizations, like we said before, AI, arthritis, the Autoimmune Foundation, arthritis Foundation, global Healthy Living Foundation.
Yes. All of these organizations do have, um, advisors that they double check and make sure that all of their resources are, um, medically reviewed and that are, um, you know. Accurate and making sure that we're creating resources that can be helpful to everybody. So definitely making sure to stay informed.
Coming back and listening to this talk show, taking a look at all of the different resources that we have, um, in our patient journey, um, section of our website can be really helpful. And they are, um, divided by the different stops of the [00:37:00] patient journey, like we said. The undiagnosed or mystery patient section, the newly diagnosed section, disease management, comorbidities, even some resources for care partners.
Um, and some, one part that's, you know, gonna be built out a lot more in 2026 is information about the road to remission. Um, and that is, that is, um, a very interesting topic that's been become a hot topic in the past year. As we're seeing it, remission can be, um, more available to a lot more patients nowadays.
So yeah. Attainable. Yeah. Yes, it's sustain, which I, you know, that was. I mean, where I am in my disease journey, I've never been in remission and probably never will get there. Um, unless some miracle of getting car T-cell therapy or, or something like that. But, um, it is, it is obtainable and there are ways, and that's kind of what I am [00:38:00] thinking about for my son trying to, you know.
Keep him positive and thinking in that way. So yeah, stay tuned for that. Absolutely. And so thank you again, Deb, for being here with me today talking about, um, all the advice for those who are newly diagnosed. Um, I really appreciate you being here and putting in some of your input. And also please thank Jacob, um, your son for also giving his, um, input because he has gone through this so recently as well.
So, um, just. Just knowing that. And also, uh, we, we don't really hear male perspectives very often on, um, when it occur to a lot of these diseases. So, um, getting that and you know, from him as well. Um, yeah, I mean there's, we've seen so many different athletes that have, you know, have had these diseases as well.
Right. Um, so just, just knowing that that is a part of life. Anybody can get these busy this, um, yeah. If anybody can, [00:39:00] um, get these a and go through that same, you know, questioning, you know, what's happening, how do I deal with this? And, um, it's all gonna be the same no matter who you are. You're gonna still have those same questions on.
How do I deal with this? And so hopefully this episode gave you some encouragement, gave you some, um, practical tips on things to take a look at when you are newly diagnosed. Like I said, I will, uh, have, make sure that we link, um, a bunch of our resources, um, in. The, um, description below, and yeah, that is a wrap for this episode.
So at Air Arthritis, we don't just represent the patient voice, we are the patient voice. And with your support, we can amplify it even further. If you found value in this talk show, please consider making a donation to help us continue producing impactful conversations, bringing all stakeholders to the table to discuss patient identified issues.
Patient infused [00:40:00] solutions so you can visit AiArthritis.org/donate to help us make a difference together. Thank you again for tuning into this episode of AiArthritis Voices 360. Um, you can find AiArthritis on all social media platforms at IF AiArthritis, and that's a wrap. We will see you here next month.
On the next episode of AiArthritis Voices three. Thank you,
AiArthritis Voices 360 is produced by the International Foundation for Autoimmune and Autoinflammatory Arthritis. Find us on the web@www.AiArthritis.org. Also, be sure to subscribe to this podcast and stay up. Today on all the latest AI, arthritis news and [00:41:00] events.
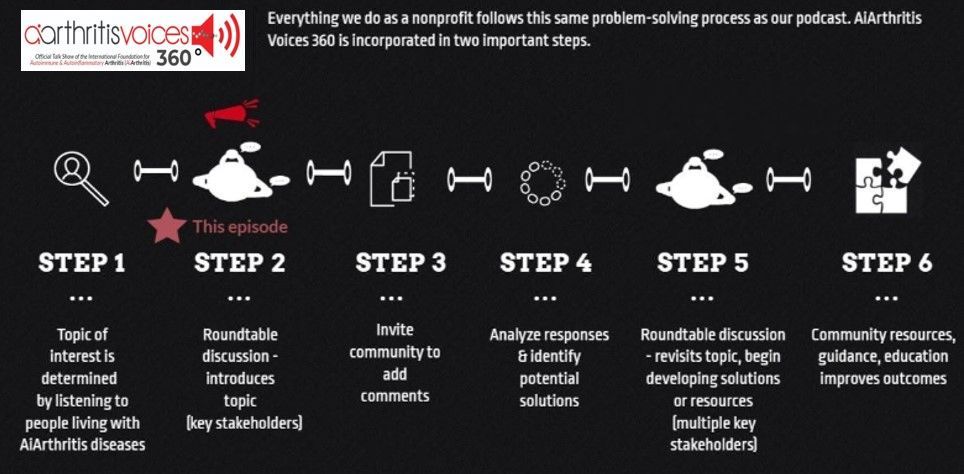
All our main 1st Sunday of the month episodes are either an initial "put the topic on the table" episode (Step 2 in our organization's 6-step problem solving process) or a "revisit to the table" episode (Step 6 in our organization's 6-step process), where we build on a past show because we have moved forward in developing help, tools, or projects around the issue (Step 5 in our organization's 6-step process).
After each show airs we spin off the conversation into many discussions over various formats, which we now call #360its.
-
Additional Resources & Information
Explore the AiArthritis Patient Journey, a resource designed to guide patients through every stage of life with autoimmune and autoinflammatory arthritis. From diagnosis to daily management, discover tools and insights to empower your journey!
Your Co-Hosts: Who is at the Table this Episode?
Leila P. L.Valete
Leila is the Health Education Manager at the International Foundation for AiArthritis. She is a person living with Lupus and Sjögren’s disease. She is passionate about inclusion and diversity in health education and meeting individuals where they are at in order to learn in a way that resonates with them.
Connect with Leila:
Tiktok: @Lupuslifestyle.lei
Deb Constien
Deb Constien is a medically retired Registered Dietitian and a Representative for the AiArthritis with Rheumatoid Arthritis. Deb is also on the Advisory Council for WREN- Wisconsin Research Education Network and a Patient Family Advisor- PFA on an International PCORI research study for ACP- Advanced Care Planning.
Connect with Deb:
- Facebook: @deb.majcherconstien
- Instagram: @debconstien
- Twitter: @debconstien
Pull up your seat at the table
Now it's YOUR TURN to join the conversation!
What do you think about this episode?
We want to know what you think! By continuing the conversation with your opinions and perspectives - we all get a better understanding of the problems facing our community. Better yet, through these conversations we can start working and developing solutions.
We mean it when say 360. Not only do we want your input anytime and anywhere, but we also are eager to see where the conversation will take us. So please, "pull up a seat at the table" and let's start talking!
Email us at podcast@aiarthritis.org, message us on social media (find us by searching for @IFAiArthritis)
Relevant Episodes & Projects
Ep. 102 - Navigating the Patient Journey: From Early Diagnosis to Remission
Info here about puppies being awesome
Ep 10: Patients Weigh In: Why the 'Right' Diagnosis Name Matters
As more treatment options are moving towards Biosimilars, many questions are being raised by patients. What are Biosimilars? Are they safe and effective? Are there downsides? Upsides? What are doctors' opinions on Biosimilars? What should I do if I am switched to a Biosimilar?
Ep. 15: Internalized Ableism: Finding Your Freedom to Participate in Life
Do biomarkers hold the key to understanding disease severity and predicting disease onset? Tiffany and Patrice discuss the importance of biomarkers & their uses for disease treatment.
Mini Ep. 4""Who Am I Now?" Finding a New Normal
Join TIffany and Rick as they address the challenges involved as Treat 2 Target has emerged from aggressive treatments for a larger population to treating per the individual and based on the complexity of each disease.
Love the show? Help us make sure we stay on the air by making a donation.
Your contribution helps us continue the work we do every day to improve the lives of millions worldwide.